Hi BKP
Not sure if you've seen this but
this Lancet piece is a compelling read. Parenthetically it's nice to see the Journals step up and make recent publications on Covid 19 public domain.
Here's my take on this - And of course one has to confess up front that at the beginning of any scientific puzzle
what you know by definition is way less than what you don't. I think the central scientific puzzle and certainly one with the greatest clinical value is the mortality puzzle –
what characterizes the highly vulnerable to those fatal outcomes. Of course everyone has jumped on the age factor, but the question is what does that mean? You may disagree with my assessment of this admittedly incomplete picture, but of course a spirited and respectful scientific debate can never be a bad thing. And preliminary hypotheses of course are always valuable because they can be falsified and then you can move on to better ideas.
I might tentatively hypothesize that the increased mortality in older groups is another finding related to the work on "inflammaging". This concept has been around for decades (and shows decisive relevance in relationship to Alzheimer's disease in my professional opinion) but in a nutshell it attempts to articulate an age-related tilt in the immune system in which upregulated and even disinhibited innate immunity Is a partial but ultimately unsuccessful compensation for declining adaptive immunity. And I believe it puts the lie to simpleminded notions about inflammation as a unidimensional volume control. It's highly differential and multicomponent, and it looks like in the patients with poorer outcomes there may be a stronger and disinhibited innate immunity response, one that's not only unsuccessful in containing the virus but that may create sepsis and organ failure. The data set in the Lancet piece of course is not conclusive for that because the only cytokine that they indexed is IL-6 which of course is one of the most important ones but they're at least another six or seven that they could've looked at. Of course this exaggerated innate immune response may emerge from greater penetration of the virus into lung and cardiac tissue (which might index another currently completely unknown vulnerability factor possibly even genotypic), and cardiac tissue looks increasingly like it's a target along with vascular tissue, as the biomarkers in the graphic below including not just troponins but also D-dimer might indicate. Intriguingly, the failing patients do not activate lymphocyte production to nearly the same degree and unfortunately they did not index B cell versus T-cell but in any case both are more involved in adaptive immunity than innate immunity. In any case and this part of course is not surprising, the poorer outcomes had sepsis and organ failure in a much higher percentage. A really tempting hypothesis is that the patients with fatal outcomes failed to mount an effective antibody response as their immune systems ramped up to the pathogen, while those with better outcomes gradually achieved increasing and viable adaptive immune resistance. In other words, patients with poor outcomes may be stuck in mostly in innate immunity response with increased damage to bystander tissues, steadily escalating pro-inflammatory cytokines and eventual sepsis, but of course this is just a speculation at this point without adequate date.
View attachment 522382
Here's the text from the article Discussion Section that's also quite informative in this regard:
"This retrospective cohort study identified several risk factors for death in adults in Wuhan who were hospitalised with COVID-19. In particular, older age, d-dimer levels greater than 1 μg/mL, and higher SOFA score on admission were associated with higher odds of in-hospital death. Additionally, elevated levels of blood IL-6, high-sensitivity cardiac troponin I, and lactate dehydrogenase and lymphopenia were more commonly seen in severe COVID-19 illness. Sustained viral detection in throat samples was observed in both survivors and non-survivors. Previously, older age has been reported as an important independent predictor of mortality in SARS and MERS.
The current study confirmed that increased age was associated with death in patients with COVID-19. Previous studies in macaques inoculated with SARS-CoV found that older macaques had stronger host innate responses to virus infection than younger adults, with an increase in differential expression of genes associated with inflammation, whereas expression of type I interferon beta was reduced. The age-dependent defects in T-cell and B-cell function and the excess production of type 2 cytokines could lead to a deficiency in control of viral replication and more prolonged proinflammatory responses, potentially leading to poor outcome.
SOFA score is a good diagnostic marker for sepsis and septic shock, and reflects the state and degree of multi-organ dysfunction. Although bacterial infections are usually regarded as a leading cause of sepsis, viral infection can also cause sepsis syndrome. Previously, we determined that sepsis occurred in nearly 40% of adults with community-acquired pneumonia due to viral infection. In the current study, we found that more than half of patients developed sepsis. Additionally, we found that more than 70% of patients had white blood cell count below 10·0 × 109 per L or procalcitonin below 0·25 ng/mL, and no bacterial pathogens were detected in these patients on admission. Sepsis was a common complication, which might be directly caused by SARS-CoV-2 infection, but further research is needed to investigate the pathogenesis of sepsis in COVID-19 illness. Cardiac complications, including new or worsening heart failure, new or worsening arrhythmia, or myocardial infarction are common in patients with pneumonia. Cardiac arrest occurs in about 3% of inpatients with pneumonia. Risk factors of cardiac events after pneumonia include older age, pre-existing cardiovascular diseases, and greater severity of pneumonia at presentation. Coronary heart disease has also been found to be associated with acute cardiac events and poor outcomes in influenza and other respiratory viral infections.
In this study, increased high-sensitivity cardiac troponin I during hospitalisation was found in more than half of those who died. The first autopsy of a 53-year-old woman with chronic renal failure in Jinyintan Hospital showed acute myocardial infarction (data not published; personal communication with a pathologist from the Chinese Academy of Science). About 90% of inpatients with pneumonia had increased coagulation activity, marked by increased d-dimer concentrations. In this study, we found d-dimer greater than 1 μg/mL is associated with fatal outcome of COVID-19. High levels of d-dimer have a reported association with 28-day mortality in patients with infection or sepsis identified in the emergency department. Contributory mechanisms include systemic pro-inflammatory cytokine responses that are mediators of atherosclerosis directly contributing to plaque rupture through local inflammation, induction of procoagulant factors, and haemodynamic changes, which predispose to ischaemia and thrombosis.
In addition, angiotensin converting enzyme 2, the receptor for SARS-CoV-2, is expressed on myocytes and vascular endothelial cells so there is at least theoretical potential possibility of direct cardiac involvement by the virus. Of note, interstitial mononuclear inflammatory infiltrates in heart tissue has been documented in fatal cases of COVID-19, although viral detection studies were not reported."
What do you think? Sorry for the long post!
It's been a while since I posted anything here, and I have to say I'm troubled that the tone of this thread has – at least at times – badly devolved. Perhaps despite our connection to Tesla which should homogenize things at least some, the thread still mirrors the deepening polarization of our country into warring tribes. Which in turn of course seems to just mirror how tribalism in its ugliest forms seems to be ascendant globally. To keep a big picture view here, we have no chance of solving the incredibly difficult challenges of climate change – and it's worth remembering that Tesla was founded in the spirit of sustainability – if we just devolve into warring tribes. We have got to start treating each other as though we are on the same team - we are all on the "human team", which is the only team status that should matter, not whether we are Chinese, or American, Italian, etc,. The Virus doesn't care about these traditional designations. Neither does a view of Earth from space, so maybe we should take our lead from that bigger picture. A discussion of why we have fulminant tribalism at this point in our history is probably subject for another thread, but the fact that people are dying, and that many tens of thousands, even many millions of lives, are still deeply at risk, clearly pours gas on the fire of our political contention/division.
If the potential fatality is part of what is driving some of the heat, let's focus on that, because I think we could really change the big picture if we could get a handle on it. If we could make this more just an unpleasant illness with minimal fatality, that would be huge. That question indexes essentially an unanswered scientific/biological puzzle, understanding how this virus is killing so many people – and as I outline below, the emphasis on
age and comorbidities isn't really an explanation but instead represents just
proxies or placeholders for a potential real explanation. I think there is a decent if not definitive scientific evidence base that both
age and comorbidities index vulnerabilities to severe and more chronic forms of inflammation of the kind generated by our immune systems in the context of a novel pathogen. One of the issues that stands out is the enormous differential effects of Covid 19, amazingly lethal for a small percentage of the population while perhaps asymptomatic for another 20+ or so percent, for whom it is no challenge at all. And although this may be true of many different types of infections, the extent of this variability is striking, and is different from many other types of infection where lethality is concentrated in
both the very old and the very young. We have to confess that this is still not very well understood. And it contrasts intensely with several other pandemics including the 1918 influenza which was often times just as lethal or more lethal for younger adults in their prime. So that's one big question and biological puzzle box – the differential lethality and symptomatology of Covid 19. One speculation of course is that the relatively asymptomatic already have a partial immunity through an previous encounter with a coronavirus relative to Covid 19. See this link to the New Yorker for an interesting non-technical review of this possibility:
Why Some Flus Are Deadliest in Young Adults.
I've had a chance to do a deeper dive on the Lancet data separating mortality from survivor cases at least in relationship to the Chinese epidemic, and compare this with other data sets including summary publications now available on the Seattle ICU data, which looks virtually identical. My prior post was admittedly too technical and probably not digestible by those without a background in medicine or in biological sciences. So I want to walk people through an evidence base for the idea that fatality in this disease may be characterized by
excessive innate immune activation and declining or somehow sluggish or otherwise at least functionally insufficient if not defective adaptive immunity, and/or that
escalating inflammation driven by innate immunity may interact with so-called comorbidities to create fatal outcomes. This second possibility has been popularized by the discussion at the CDC of a meme that a lot of people may be dying “
with coronavirus but not from coronavirus”. This reminds me a bit of the legal concept that irregardless of whether the plate was cracked before you dropped it, when it falls to the floor and breaks, you're still responsible.
Ultimately, this distinction between dying with Covid 19 versus dying from Covid 19 may be a specious distinction even mechanistically, if the common denominator between serious immunochallenge from a novel pathogen and various classic “comorbidities” is the potentially destructive effects of a chronic disinhibition of innate immunity. This includes overwhelming evidence of solid mechanistic connections between disinhibited innate immunity/chronic inflammation and most if not all of the classic diseases of aging now considered "comorbidities" in the Covid 19 fatality math: 1)
coronary artery disease and atherosclerosis; 2)
type II diabetes; 3)
many if not most cancers; 4)
most if not all neurodegenerative disorders but most certainly Alzheimer's disease.
This notion of declining adaptive immunity with a partially compensatory but ultimately maladaptive upregulation of innate immunity is a concept that's been around for a fairly long time (first articulated by an Italian researcher), referred to as "inflammaging" – and I became familiar with it in my decades-long struggle trying to understand the biological puzzle box of Alzheimer's disease where this concept potentially explains a number of the paradoxes of AD and provides Insights that may improve our currently rather poor treatment options for that disease. I thought I recognized the signature of 'inflammaging' in the Lancet data almost immediately, but I wanted to develop this in a way that any smart, curious lay person can follow.
One of the issues in 'inflammaging' is that not only is the transition to adaptive immunity more sluggish but there's also a modest but intrinsic competition between these branches of the immune system, something rarely appreciated in general medicine - in this sense, an overwhelming innate immunity response can actually inhibit the potential transition to a successful adaptive immunity (this is the type of more targeted and therefore less self-destructive immunity mediated by antibodies and various lymphocytes).
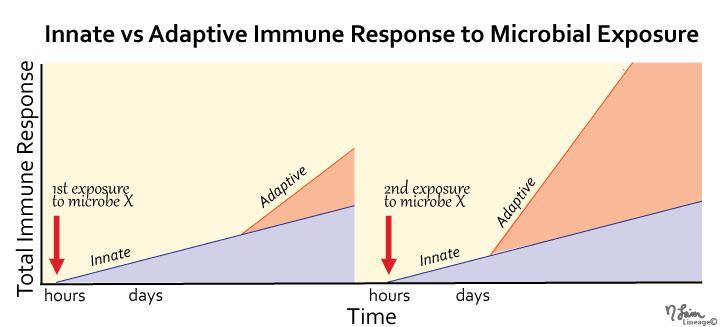
This means that folks who cannot mount effective adaptive immunity - which should be the transitioning (after 7-10 days or so) and constituting the tail end of their immune response to this pathogen (and all novel pathogens with which we have no experience) - instead mount an increasingly disinhibited innate immunity campaign, with sepsis and lethal consequences as a potential trajectory. This can be indexed with steadily rising pro-inflammatory cytokines sometimes rather colloquially referred to as a "cytokine storm" or more technically as "cytokine release syndrome".
For folks not familiar with the adaptive vs innate branches of the immune system, here's several neat little graphics that give some insights into this critical distinction. Adaptive immunity appeared in the vertebrate line of evolution a long time ago and it gave a crucial advantage over innate immunity in terms of a more targeted and less self-destructive response along with the ability to learn pathogens so that an early and effective antibody-mediated campaign can be waged against the now-recognized returning invader instead of waiting for a generalized pro-inflammatory reaction that again potentially harms a lot of "bystander tissues".
Although it is still somewhat controversial and incompletely understood in terms of the biological dynamics of sepsis and septic shock, past a certain point a
generalized pro-inflammatory state threatens life itself. It certainly causes altered mental status (as part of so called "sickness behavior" effects emerging directly from cytokines), fever (as an innate immunity defensive response orchestrated by cytokine-hypothalamic interactions), progressive physical and mental incapacity and eventually coma. Death in Covid 19 may take place because extremely high levels of inflammation eventually disrupt cardiac and respiratory physiologic function, (probably due to combined effects of both the virus and our immune system), including a nontrivial risk of MI from virus-immune interactions destabilizing plaques (not coincidentally one of the major interferons (interferon gamma) actually destabilizes plaque structures and turns them into floating clot bombs).
In part 2 of this overly long post, I'm going to unpack the Lancet ICU data from the Chinese Covid 19 summary showing how all this data may fit with the hypothesis of disinhibited innate immunity and sluggish or deficient adaptive immunity.
This graphic makes it clear that T cells and B cells (different forms of lymphocytes) are the critical orchestrators of adaptive immunity, and are recruited by dendrite cells that serve as bridge macrophages linking innate and adaptive immunity. Not pictured in this graphic is how antibodies chemically attach to pathogens, and then serve as a homing signal for various macrophages and killer cells. A central immunologic problem in aging is that we seem to be unable to replenish so-called naïve T cells (which are necessary to learn a novel pathogen), as there are fewer and fewer of them decade by decade. Additionally, and increasing population of our cells as we hit our 70s and 80s are “
senescent” which means that they cannot divide and replicate. Additionally those senescent populations release (on their own and unbidden so to speak) an increasing number of pro-inflammatory cytokines even without presentation of pathogens to various innate immunity receptors. It's interesting that our innate immune systems are capable of recognizing fungi, bacteria, and many viruses, simply by virtue of their characteristic proteins and other molecular signatures, through so-called PRRs, or
Pathogen
Associated
Molecular
Pattern receptors. This makes it clear that we have been in a battle with these other more ancient life forms through the eons of deep evolutionary time. The memory of that battle so to speak is in our innate immune system. Our adaptive immune system provides us with a more chronologically recent and individual memory system for preserving a record of and targeted defense against specific pathogens, over and above what is encoded in the receptor system supporting innate immunity. Successful resolution of most viral infections appears to require the adaptive immune system to come on board and do much of the final mop up so to speak. The innate immune system by itself may not be enough.
The treatment implications for this are obvious, that convalescent plasma with its IgG antibodies may be our best bet for a disease-modifying therapy, although we have to be sure that we are not swapping one massive immunochallenge for another, but that should be fairly easy as we have a long track record of pretty good success with convalescent plasma. I'm also modestly encouraged by some of the more recent but still not definitive reports about chloroquine and hydroxychloroquine. In the meantime we have to do social distancing and other classic forms of mitigation to prevent ICUs/our supply of ventilators from being totally overwhelmed. Respiratory support will allow a lot of seriously ill people to survive, but if we can't provide that Due to the system surge overwhelming capacity, the case fatality rate goes from probably under 1% to whatever our ICU and critical care percentage of infection might be.
And that's a hell of a lot more than 1%.


